What is the pathophysiology of hypoglycemia
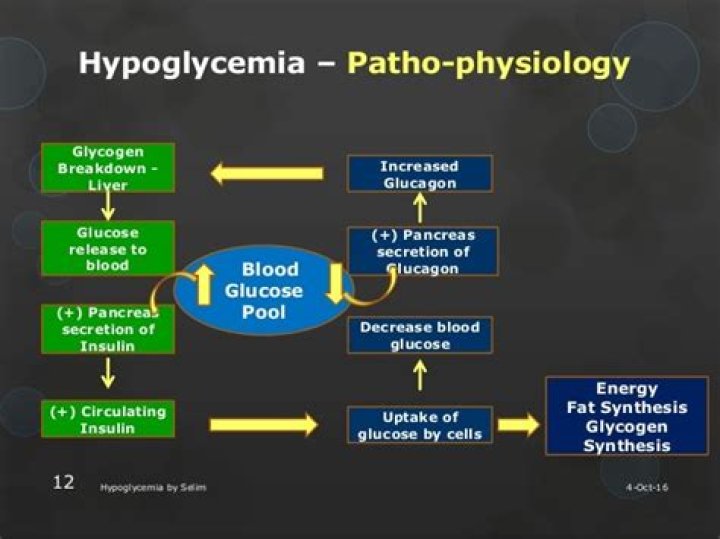
Hypoglycemia is characterized by a reduction in plasma glucose concentration to a level that may induce symptoms or signs such as altered mental status and/or sympathetic nervous system stimulation. This condition typically arises from abnormalities in the mechanisms involved in glucose homeostasis.
What is the pathophysiology of hyperglycemia?
Hyperglycemia results from a decrease in the body’s ability to utilize or store glucose after carbohydrates are ingested and from an increase in the production of glucose by the liver during the intervals between meals.
What is a pathological indicator of hypoglycemia?
More severe hypoglycemia—for example, blood glucose concentrations less than 45 mg per 100 ml (2.5 mmol/l)—causes blurred vision, impaired thinking and consciousness, confusion, seizures, and coma. These symptoms are known as neuroglycopenic symptoms because they are indicative of glucose deprivation in the brain.
What are the common physiological causes of hypoglycemia?
- Taking too much insulin or diabetes medication.
- Not eating enough.
- Postponing or skipping a meal or snack.
- Increasing exercise or physical activity without eating more or adjusting your medications.
- Drinking alcohol.
What is the pathophysiology of glucose?
The rise in blood glucose levels signals important cells in the pancreas, called beta cells, to secrete insulin, which pours into the bloodstream. Within 20 minutes after a meal insulin rises to its peak level. Insulin enables glucose to enter cells in the body, particularly muscle and liver cells.
What is Type 2 diabetes pathophysiology?
The pathophysiology of type 2 diabetes mellitus is characterized by peripheral insulin resistance, impaired regulation of hepatic glucose production, and declining β-cell function, eventually leading toβ -cell failure.
What happens in the body during hypoglycemia?
Because the brain depends on blood sugar as its primary source of energy, hypoglycemia interferes with the brain’s ability to function properly. This can cause dizziness, headache, blurred vision, difficulty concentrating and other neurological symptoms.
What conditions can cause hypoglycemia?
- Drinking too much alcohol. When a person’s blood sugar levels are low, the pancreas releases a hormone called glucagon. …
- Medication. …
- Anorexia. …
- Hepatitis. …
- Adrenal or pituitary gland disorders. …
- Kidney problems. …
- Pancreatic tumor.
How does hypoglycemia cause seizures pathophysiology?
The data indicate that the seizures noted early in the course of insulin-induced hypoglycemia are temporally related to a rise in brain osmolality secondary to an increased net transport into brain of Na+ and K+, probably caused by insulin, per se.
What causes hypoglycemia in non diabetics?The underlying cause of nondiabetic hypoglycemia varies. Sometimes it’s due to an imbalanced or unhealthy diet. You receive glucose (which is your body’s main energy source) from food. Therefore, you might experience a drop in blood sugar after going several hours without food or if you don’t eat before a workout.
Article first time published onWhat is the root cause of hypoglycemia?
Hypoglycemia is most often caused by drugs taken to control diabetes. Much less common causes of hypoglycemia include other drugs, critical illness or organ failure, a reaction to carbohydrates (in susceptible people), an insulin-producing tumor in the pancreas, and some types of bariatric (weight loss) surgery.
What is the most common pathological indicator of hypoglycemia?
- Shaking, trembling or weakness.
- Sweating.
- Paleness.
- Hunger.
- Light headedness.
- Headache.
- Dizziness.
- Pins and needles around mouth.
Is hypoglycemia a diagnosis?
Fasting or reactive hypoglycemia is diagnosed by a blood test to measure blood glucose. The test may be performed after fasting overnight, physical activity, or between meals.
What pathophysiology means?
Definition of pathophysiology : the physiology of abnormal states specifically : the functional changes that accompany a particular syndrome or disease.
What do you write in pathophysiology?
The page name should be “(Disease name) pathophysiology”, with only the first letter of the title capitalized. Goal: to explain the biological mechanisms underlying the disease state.
What is the pathophysiology of diabetes insipidus?
Diabetes insipidus is caused by abnormality in the functioning or levels of antidiuretic hormone (ADH), also known of as vasopressin. Manufactured in the hypothalamus and stored in the pituitary gland, ADH helps to regulate the amount of fluid in the body.
What are hypoglycemic hormones?
Glucagon helps your liver break down the food you eat to make glucose. If your blood sugar drops too low, you can get hypoglycemia.
What organs are affected by hypoglycemia?
The brain is one of the first organs to be affected by hypoglycemia. Shortage of glucose in the brain, or neuroglycopenia, results in a gradual loss of cognitive functions causing slower reaction time, blurred speech, loss of consciousness, seizures, and ultimately death, as the hypoglycemia progresses.
What happens to the brain during hypoglycemia?
Hypoglycemia commonly causes brain fuel deprivation, resulting in functional brain failure, which can be corrected by raising plasma glucose concentrations. Rarely, profound hypoglycemia causes brain death that is not the result of fuel deprivation per se.
What is the physiological difference between Type 1 and 2 diabetes?
Type 1 diabetes is an autoimmune disease. It occurs when the insulin-producing islet cells in the pancreas are completely destroyed, so the body can’t produce any insulin. In type 2 diabetes, the islet cells are still working. However, the body is resistant to insulin.
What are the 3 types of diabetes mellitus?
- Type 1 Diabetes. Type 1 diabetes is thought to be caused by an autoimmune reaction (the body attacks itself by mistake) that stops your body from making insulin. …
- Type 2 Diabetes. …
- Gestational Diabetes.
What are the causes of diabetes explain?
What causes type 1 diabetes? Type 1 diabetes occurs when your immune system, the body’s system for fighting infection, attacks and destroys the insulin-producing beta cells of the pancreas. Scientists think type 1 diabetes is caused by genes and environmental factors, such as viruses, that might trigger the disease.
What is a hypoglycemic seizure?
Possible Complications. Expand Section. Severe low blood sugar is a medical emergency. It can cause seizures and brain damage. Severe low blood sugar that causes you to become unconscious is called hypoglycemic or insulin shock.
How does hypoglycemia affect EEG?
The EEG presentation of hypoglycemia involves low frequency and increased amplitude of delta to theta activity. It is known that these EEG patterns are not correlated with altered consciousness or sleep in patients with hypoglycemia.
Which one induce the seizure hyperglycemia or hypoglycemia?
Diabetes is the most common cause of the seizures in patients with low blood glucose.
What causes hypoglycemia in the morning?
A person who takes insulin doesn’t eat a regular bedtime snack, and the person’s blood sugar level drops during the night. The person’s body responds to the low blood sugar by releasing hormones that raise the blood sugar level. This may cause a high blood sugar level in the early morning.
Can anemia cause hypoglycemia?
Point-of-care (POC) blood glucose analysis is standard; however anemia causes falsely high values and potentially masks hypoglycemia. Permissive anemia is routinely practiced in most intensive care units (ICUs).
How does hypoglycemia induce glucagon production?
Normally, a decrease in the plasma glucose concentration causes a decrease in β-cell insulin secretion that signals an increase in α-cell glucagon secretion during hypoglycemia.
How do nurses treat hypoglycemia?
Nursing management includes administering glucose tablets (approximately three), glucose gel, or carbohydrates for the conscious patient. Carbohydrates may consist of 4 to 6 ounces of fruit juice or soda (not sugar-free), saltine crackers, or hard candy (only if the patient is alert).
How does glucagon treat hypoglycemia?
That’s why glucagon is available as a medication to assist in cases of severe hypoglycemia, when a person isn’t able to treat themselves. Glucagon medication triggers the release of glucose from the liver to increase blood sugar levels, just as the natural hormone is supposed to do.
What test is done for hypoglycemia?
To check for reactive hypoglycemia, you may have to take a test called a mixed-meal tolerance test (MMTT). For this, you take a special drink that raises your blood glucose. The doctor will check your blood glucose levels over the next few hours.